Guidong’s Fight: A Diary of Caring for My 15-Year-Old Chihuahua Through Pancreatitis
I’ve been putting off writing this. Partly because it’s hard to find the right words, and partly because every time I sit down to type, I end up just staring at Guidong sleeping on his blanket instead. But I think this story needs to be told — for anyone else out there sitting in a vet’s waiting room with a senior dog, heart pounding, hoping for the best.
Guidong is my 15-year-old Chihuahua. Fifteen. That’s a whole lifetime in dog years, and honestly, he’s been my whole lifetime too. So when the test results came back two weeks ago, it felt like the ground dropped out from under me.
Day 1: The Numbers That Changed Everything
I knew something was wrong when Guidong stopped eating. This is a dog who has never, in fifteen years, turned down food. Not once. So when he just looked at his bowl and walked away, I grabbed my keys and drove to the vet before I could even think about it.
The blood work came back, and I wish I could say I understood what I was looking at. I didn’t. But the vet’s face told me everything I needed to know before she even started explaining.


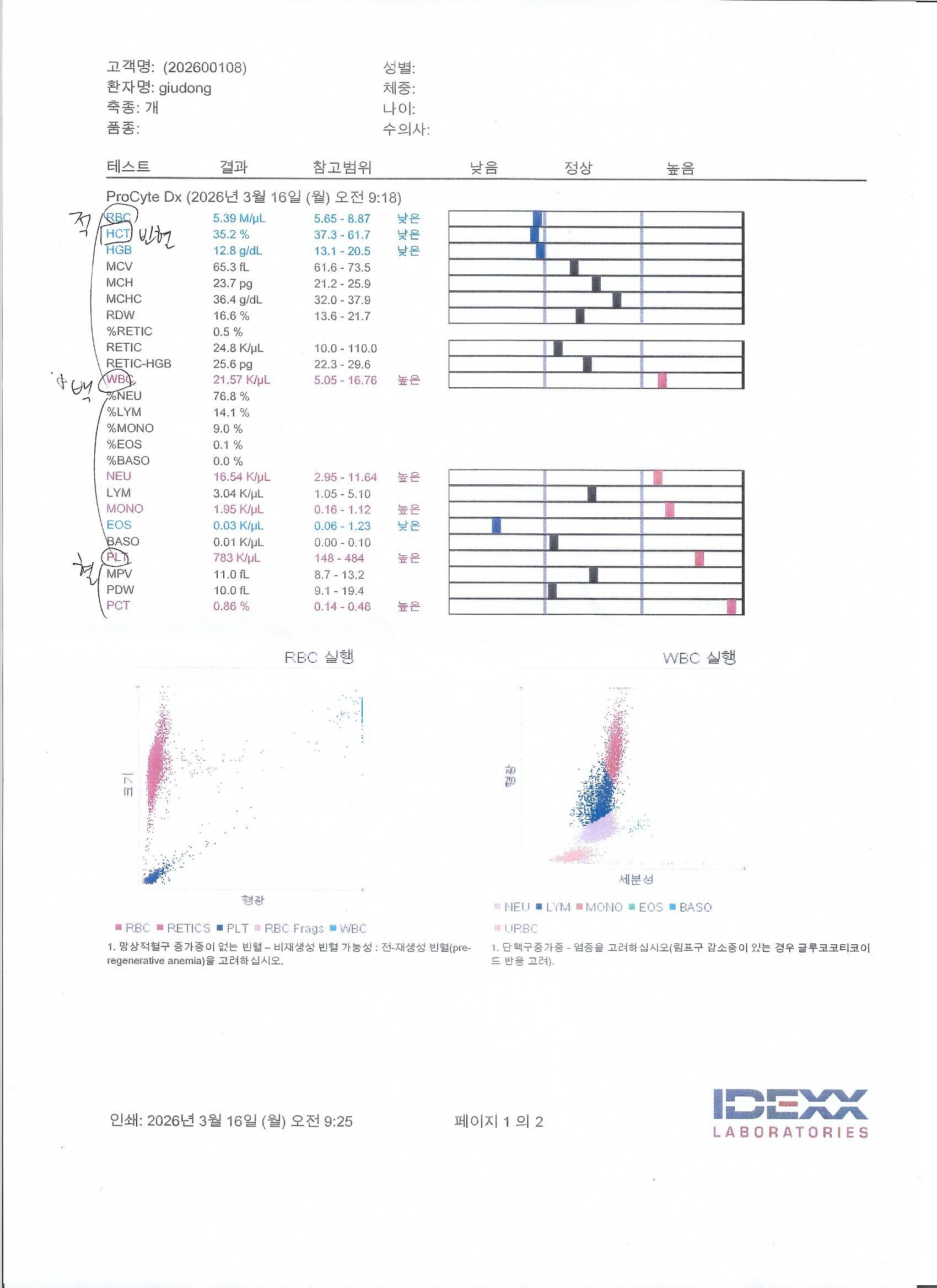
Here’s what the numbers said:
- CRP (inflammation): 5.4 mg/dL — Normal is under 1.0. His body was fighting something massive.
- Pancreatic lipase: 1,261 U/L — Normal tops out at 200. Acute pancreatitis, no question.
- ALKP (liver): 1,617 U/L — Should be under 212. The vet mentioned possible liver tumor and bile stasis.
- BUN (kidney): 54 mg/dL — Elevated. Kidney function declining, likely complicated by dehydration.
- WBC: 21.57 K/uL — White blood cells through the roof, his immune system in overdrive.
The vet’s summary hit hard: severe pancreatitis with gastritis, suspected liver tumor, kidney cysts. Vomiting, pain, hypothermia. I sat in my car for twenty minutes before I could drive home.
Day 2: The Smallest Miracle
I barely slept that night. I set alarms every two hours to check on him, adjust his blanket, make sure he was still breathing. (I know. I know. But you’d do the same.)
And then, around 7am, something incredible happened. He walked to his food bowl. On his own. And he ate.
It wasn’t much — a few bites of the prescription i/d Low Fat food I’d mixed with steamed cabbage and carrots. But watching him eat felt like watching a sunrise after the longest night of my life. I stood there in the kitchen crying into my coffee like an idiot, and I didn’t care.
The food plan became my obsession:
- Base: Hill’s i/d Low Fat prescription diet — gentle on the pancreas
- Cabbage: Steamed until very soft, for gut lining protection
- Carrots: Steamed and finely chopped, for antioxidants to support liver health
- Rule: Everything boiled or steamed, never fried or raw. Tiny portions, 4-5 times a day. Watch his face after every bite.
Day 3: Good News and Bad News Walk Into a Vet’s Office
Two days later, back at the vet for follow-up blood work. I’d been oscillating between cautious optimism (he ate breakfast!) and catastrophic thinking (what if this is the last time he eats breakfast?) all morning.
The results were… mixed. Which, if you’ve ever dealt with a sick senior pet, you know is pretty much the standard emotional rollercoaster.
- CRP dropped — The inflammation was responding to treatment. The vet said we’d “turned a corner.” I wanted to hug her.
- Pancreatic lipase rose to 1,979 — Wait, what? The pancreatitis was actually getting worse even as the overall inflammation improved. The vet explained this isn’t uncommon; the pancreas can flare before it settles.
- Liver enzymes still sky-high — ALT at 161, ALKP at 1,488. The tumor (if that’s what it is) wasn’t going anywhere.
The vet gently brought up the option of a specialist hospital. CT scans. Maybe surgery. And I had to sit with the hardest question I’ve ever faced: do I put a 15-year-old dog through general anesthesia and invasive procedures?
I decided no. Not because I don’t love him enough to try everything — God knows I’d sell my car if it would help — but because I love him enough to choose his comfort over my need to feel like I’m “doing everything.” Our vet agreed. Quality of life over quantity. Supplements, careful diet, pain management, and all the love in the world.
Day 4: The Setback (and What It Taught Me)
Just when I thought we’d found our rhythm, 10:30am happened. Diarrhea. Out of nowhere.
I’d started him on an iron supplement that morning (for the mild anemia) plus a new kidney support medication. Two and a half hours later, his gut said absolutely not.
After some panicked googling and a call to the vet, here’s what we figured out:
- Iron supplements are notoriously harsh on the stomach — and his stomach was already a war zone from the pancreatitis
- We paused the iron immediately
- Kidney meds: keeping them but adjusting timing per vet advice
- Food strategy: stripped back to prescription diet only, no vegetables for now, absolute simplicity until his gut stabilizes
Lesson learned: with a senior dog this fragile, you change one thing at a time. Not two. Not three. One. And you wait. Patience isn’t just a virtue here — it’s medicine.
Day 10: The Follow-Up (March 26)
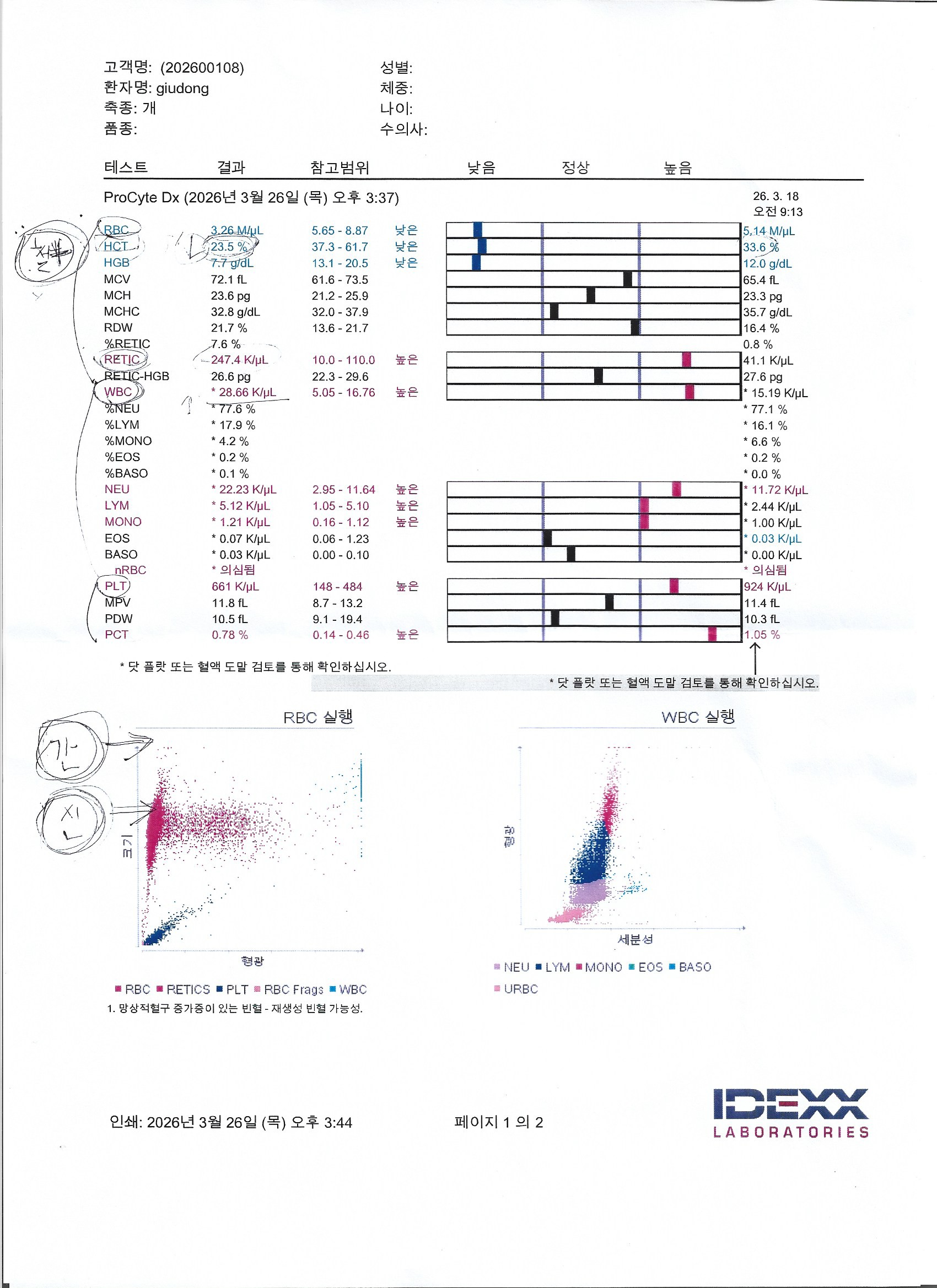
Ten days in, another round of blood work. I’ve gotten weirdly good at reading these charts now. The numbers are still far from normal, but the trend matters more than any single number. And the trend is… cautiously okay. He’s eating. He’s walking to his water bowl. Yesterday he wagged his tail when I came home, and I had to sit down because my knees went weak.
What I’ve Learned (So Far)
I’m not a vet. I’m just someone who loves his dog more than he knows how to express. But if you’re going through something similar, here’s what I wish someone had told me on Day 1:
- The numbers aren’t the whole story. A dog with terrible blood work who eats, walks, and wags is doing better than the numbers suggest. Watch your dog, not just the chart.
- “Doing everything” isn’t always the kindest choice. Sometimes the bravest thing is choosing comfort over aggressive treatment. That’s not giving up. That’s love.
- Food is medicine. A careful, low-fat, easily digestible diet made a visible difference within days. Talk to your vet about prescription diets.
- One change at a time. Senior dogs on multiple medications are fragile systems. Introduce things slowly and watch closely.
- It’s okay to cry in your car. Or your kitchen. Or the vet’s office. The staff have seen it all, and they get it.
Guidong is asleep on his favorite blanket as I write this. His breathing is steady. His belly is full of prescription kibble. And tomorrow, we’ll do it all again — the meds, the careful meals, the watching, the hoping. One day at a time.
If you’re caring for a senior dog right now, I see you. It’s exhausting and heartbreaking and beautiful all at once. You’re doing a good job. They know.
Disclaimer: I’m sharing our personal experience, not medical advice. Every dog is different. Always work with your veterinarian to determine the best treatment plan for your pet.